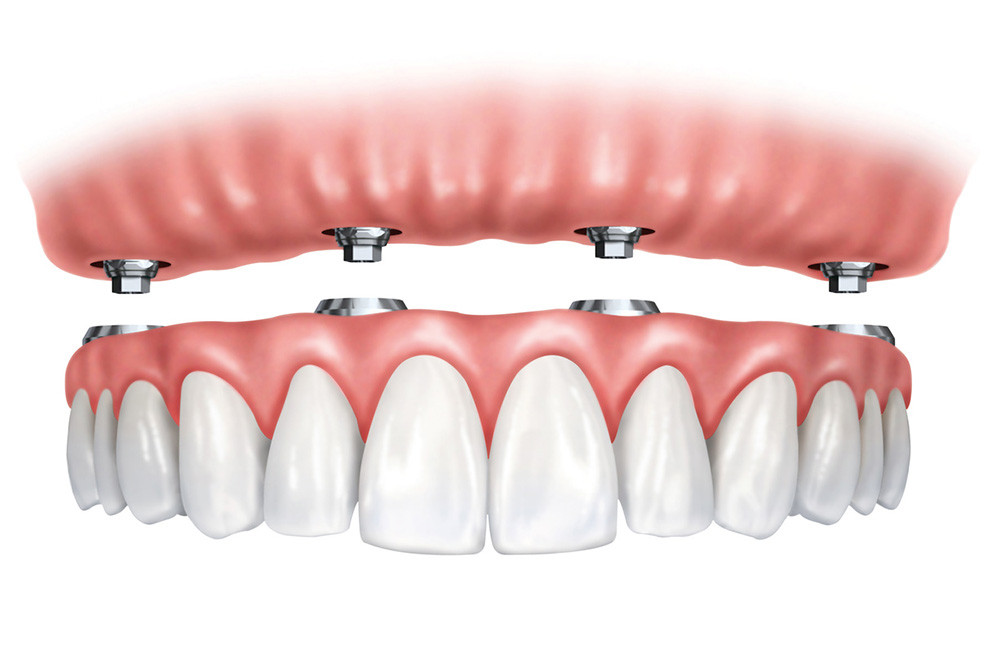
The most recent therapeutic protocols, combined with modern technologies, allow very minimally invasive implant therapies for the patient and reduced treatment times.
The advantages offered by these new treatment modalities are certainly accentuated in the therapy of the completely edentulous patient who suffers from aesthetic, functional, nutritional and psychosocial problems.
The elements that revolutionized the old therapeutic protocols were: immediate loading, guided surgery and conscious sedation.
Immediate loading refers to the possibility of immediately using the implants to support a temporary prosthesis without waiting for the traditional 4/6 months from the moment of installation.
This means that patients with mobile prostheses can immediately replace the denture with a fixed prosthesis and patients not wearing mobile prostheses, but with failing dentition, also may have the possibility having an immediate fixed implant-supported prosthesis.
This procedure is practicable in many clinical situations in relation to the quantity and quality of the residual bone.
Guided surgery is certainly the most significant innovation that has impacted implantology in recent years.
This tool allows you to make a virtual design of the implant treatment, evaluating the patient’s bone anotomy with extreme precision in relation to the individual prosthetic parameters.
Firstly, it is a diagnostic tool of great importance in favour of patient safety and adequate planning.
Once the planning and design phase is finished, a surgical template will allow the dentist to place the implants in the patient’s mouth, according to the design already predetermined on the computer, and then finally the temporary fixed prosthesis built before the operating phase will be put in.
If the bone anatomy permits, the implant installation can take place without the opening of a surgical flap and therefore, once the therapy is completed, even stitches will not be necessary.
Conscious sedation is an anesthesiological technique that involves controlling the patient’s psycho-emotional component, thus reducing anxiety and its consequences at a cardiovascular level.
It has to be done by an anesthesiologist and it offers the advantage of relaxing and monitoring the patient during the procedure. Little quantities of anxiolytic drugs are administered intravenously. It does not alter the patient’s state of consciousness but it does lessen the effects of tension.
Blood pressure stabilization on resting values is obtained. The complications that often present such as excess salivation, stimulation of vomiting and difficulty in maintaining the position required by the dentist are consequently eliminated. The patient is monitored for greater safety of the operation. All post-operative complications such as pain and swelling are also almost eliminated.
Although the patient is able to leaves the studio unaccompanied, they must not drive bikes, motorbikes and cars for the first 4 hours after their surgery.
This protocol is particularly effective in treating PHOBIC PATIENTS or PATIENTS WITH SYSTEMIC PATHOLOGIES, as the complete monitoring of the patient during the procedures and the possibility of administering intravenous drugs, if necessary, allows you to intercept and promptly manage any complications.
The enormous advantages offered by this anesthesiological approach have prompted us to extend this method of working also onto patients who: are in good health, not phobic, and candidates for invasive and / or long-lasting surgical therapies. In this way, the patient has better operative and post-operative comfort.